Prior Authorization
WHAT TO KNOW
What is Prior Authorization?
Before a patient can receive a particular prescription medication, doctors must submit information to the insurance company detailing the patient’s specific need for the medication. Once the insurance company has received the doctor’s justification, they will approve the medication and the patient can receive his or her treatment.
What is the purpose of Prior Authorization?
Prior authorization is a tactic that insurance companies use to contain health care spending. Insurance companies apply prior authorization procedures to certain high cost medications. They do this to ensure that a prescription is medically necessary before agreeing to pay for it.
Does the current system of Prior Authorization hurt patients?
Yes. Many patients incur a long waiting period before they begin necessary medications.
Doctors are frustrated by the system and it is a tedious/confusing process to navigate.
-
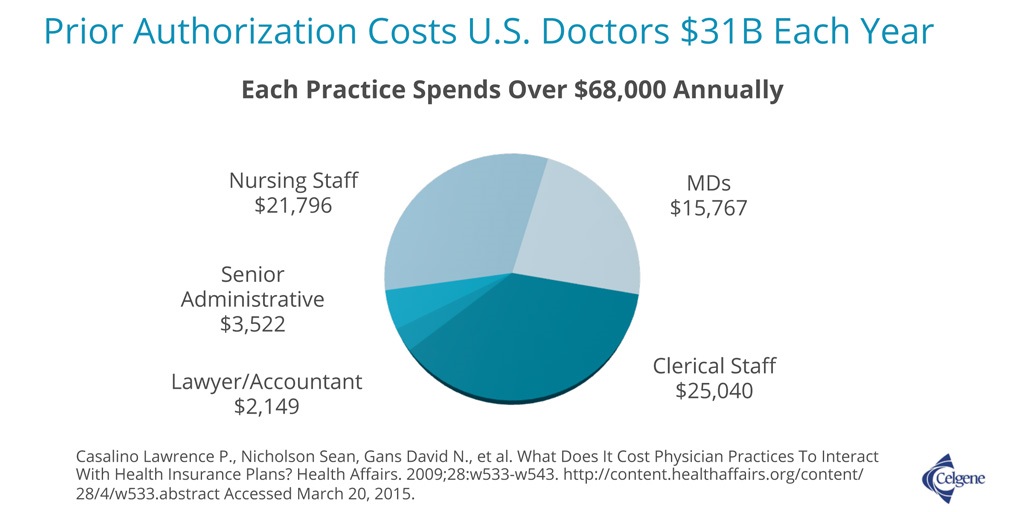
According to a recent study, the average physician practice devoted 1 hour of physician time, 13.1 hours of nursing time and 6.3 hours of clerical time to the prior authorization process each week 1.
A streamlined system would ensure timely treatment for patients and physicians’ time devoted less to paperwork and more to direct patient care.
What does prior authorization legislation try to accomplish?
The type of legislation we advocate for is aimed at implementing a streamlined and standardized process to submit prior authorization information and shorten the time between when a patient is prescribed a medicine and when they begin treatment.
According to a recent study, the average physician practice devoted 1 hour of physician time, 13.1 hours of nursing time and 6.3 hours of clerical time to the prior authorization process each week 1.
This video by Inland Empire Health Plans in California helps explain the Prior Authorization process. The process is similar for other Private health plans.
WHAT TO SAY
Your talking points
LEARN MORE
This profile will be able to show you a current outlook for States that are currently considering or have recently passed legislation regarding Step Therapy. If you live in one of the highlighted states, get in touch with your local representatives and explain to them why these bills need their support. If you live in a state that is not highlighted, you must explain to your local representatives why they should draft this type of legislation and the positive impact it would have on people like you. We at GHLF are happy to help you prepare those comments if you need assistance.
Specialty Tier Drugs