Non-Medical Switching
WHAT TO KNOW
Why do insurance companies use non-medical switching?
In the modern healthcare environment, insurance companies regularly review and change coverage tiers and policies regarding specialty medications, or ‘biologic’ drug coverage.
When prescription drug coverage changes are made, insurance companies notify patients that they may need to switch medications to one less expensive(based on how they’ve evaluated and reorganized their drug coverage policies) to avoid an increase in out-of-pocket costs. This is known as “non-medical switching”.
Can non-medical switching harm patients?
Yes, unnecessary medication switches can erode patient health & increase costs.
When dealing with patients who have complex, chronic, or rare conditions, changing a stable patient’s medication put the patient’s health at risk, potentially causing adverse side effects and decreased effectiveness of their medication. One recent study of Crohn’s Disease patients found that switching from one therapy to another was associated with loss of effectiveness within one year.
For a patient on a biologic medication, a switch can result in immunogenicity, which is an immune response that can lead to a severe allergic reaction and potentially cause patients to no longer respond to therapy.
These unintended health consequences translate to increased ER visits, hospitalizations, physician visits and lab tests – which also drive up health care costs.
This video will help explain Non-Medical Switching
WHAT TO SAY
Your talking points
States need legislation to protect commercial patients with complex, chronic, and rare medical conditions from non-medical switching practices by commercial health plans and PBMs. State laws governing commercial health plans and PBMs must be changed to ensure the following:
LEARN MORE
This profile will be able to show you a current outlook for States that are currently considering or have recently passed legislation regarding Step Therapy. If you live in one of the highlighted states, get in touch with your local representatives and explain to them why these bills need their support. If you live in a state that is not highlighted, you must explain to your local representatives why they should draft this type of legislation and the positive impact it would have on people like you. We at GHLF are happy to help you prepare those comments if you need assistance.
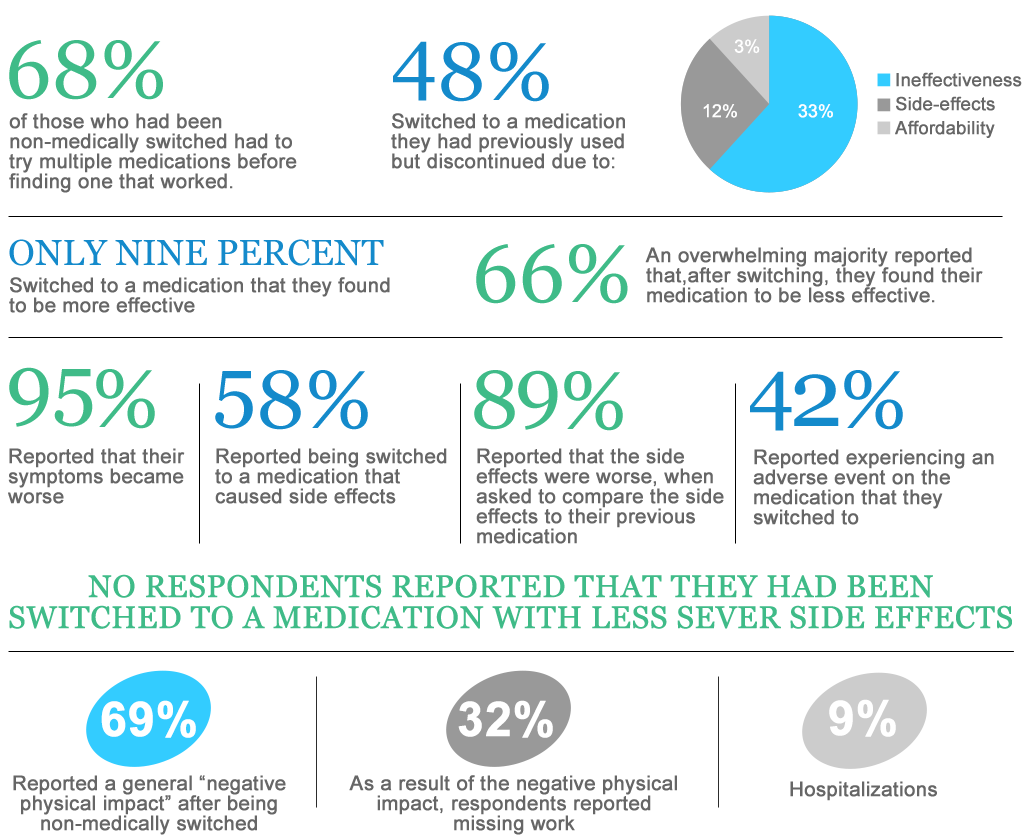
How does non-medical switching impact patient’s treatment and health?