Fail First / Step Therapy
WHAT TO KNOW
What is Fail First/Step Therapy
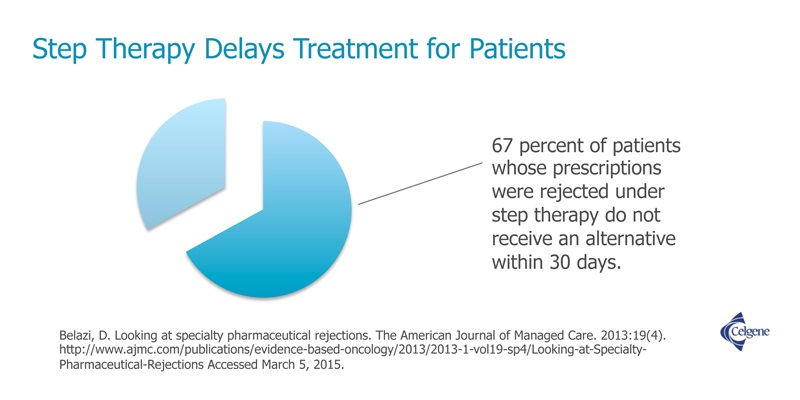
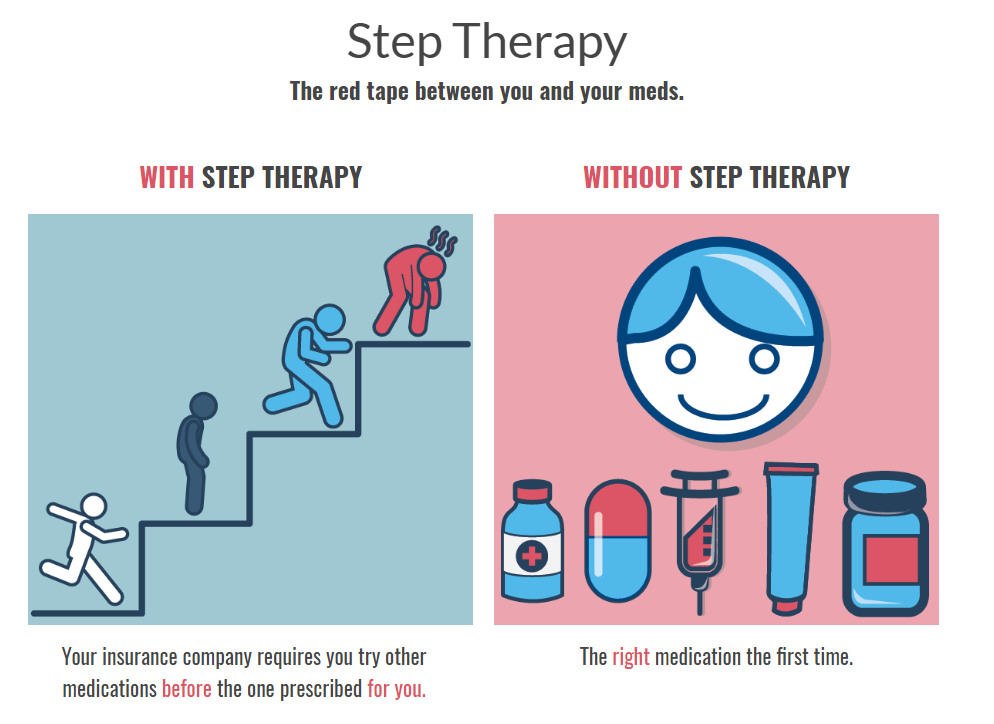
Fail First policies — also known as Step Therapy — are often insurance practices which require patients to fail on the insurer’s preferred drug, or drugs, before a patient can take the drug originally prescribed. Sometimes the preferred drugs are cheaper to the patient and sometimes they are not. Insurers can make a higher profit on the drugs they force patients to step through, and this is sometimes why they implement the policy. , Other times, fail first represents a generic drug which can be cheaper for the patient and less profitable for the insurer. However, your physician should make this decision, not your health insurance company.
Why would insurance companies use Fail First/Step Therapy?
Fail First/Step Therapy policies are used by health insurers to control costs. However, they are time-consuming from a physician and patient standpoint and are more expensive from a direct and indirect out-of-pocket cost perspective. The practice denies patients the drugs they need when they need them, and allows insurance companies to practice medicine without a license. And, while fail first policies control costs, the savings do not result in lower premiums for you. Instead they produce higher profits for insurance companies.
Can Fail First/Step Therapy harm patients?
Yes, these policies have already hurt patients severely in some states. If we do not speak out against the practice, Fail First/Step Therapy will continue to impact patients by:
-
-
Creating additional barriers that can lead people to forgo needed medications
-
Causing patients’ medical conditions to deteriorate, increasing the need for medical intervention in the future and raising the cost of health care
-
Increasing frustration and incidents of depression
-
Increasing the risk of non-compliance and self-medication.
-
Creating additional barriers that can lead people to forgo needed medications
-
Causing patients’ medical conditions to deteriorate, increasing the need for medical intervention in the future and raising the cost of health care
-
Increasing frustration and incidents of depression
-
Increasing the risk of non-compliance and self-medication.
WHAT TO SAY
Your talking points
LEARN MORE
This profile will be able to show you a current outlook for States that are currently considering or have recently passed legislation regarding Step Therapy. If you live in one of the highlighted states, get in touch with your local representatives and explain to them why these bills need their support. If you live in a state that is not highlighted, you must explain to your local representatives why they should draft this type of legislation and the positive impact it would have on people like you. We at GHLF are happy to help you prepare those comments if you need assistance.
Specialty Tier Drugs